Why Choosing the Right Mental Health Billing Services Company in the USA Can Transform Your Practice
The mental health landscape in the USA is evolving rapidly. With increasing awareness, growing patient volumes, and changing insurance regulations, providers are under more pressure than ever—not just clinically, but administratively. One of the most persistent challenges? Billing.
If you’re a therapist, psychologist, or behavioral health provider, you already know that billing isn’t just paperwork—it’s the backbone of your revenue. That’s where a reliable mental health billing services company becomes essential.
This article breaks down how specialized billing support can reshape your practice, improve collections, and give you back the time you actually want to spend with patients.
The Rising Complexity of Mental Health Billing
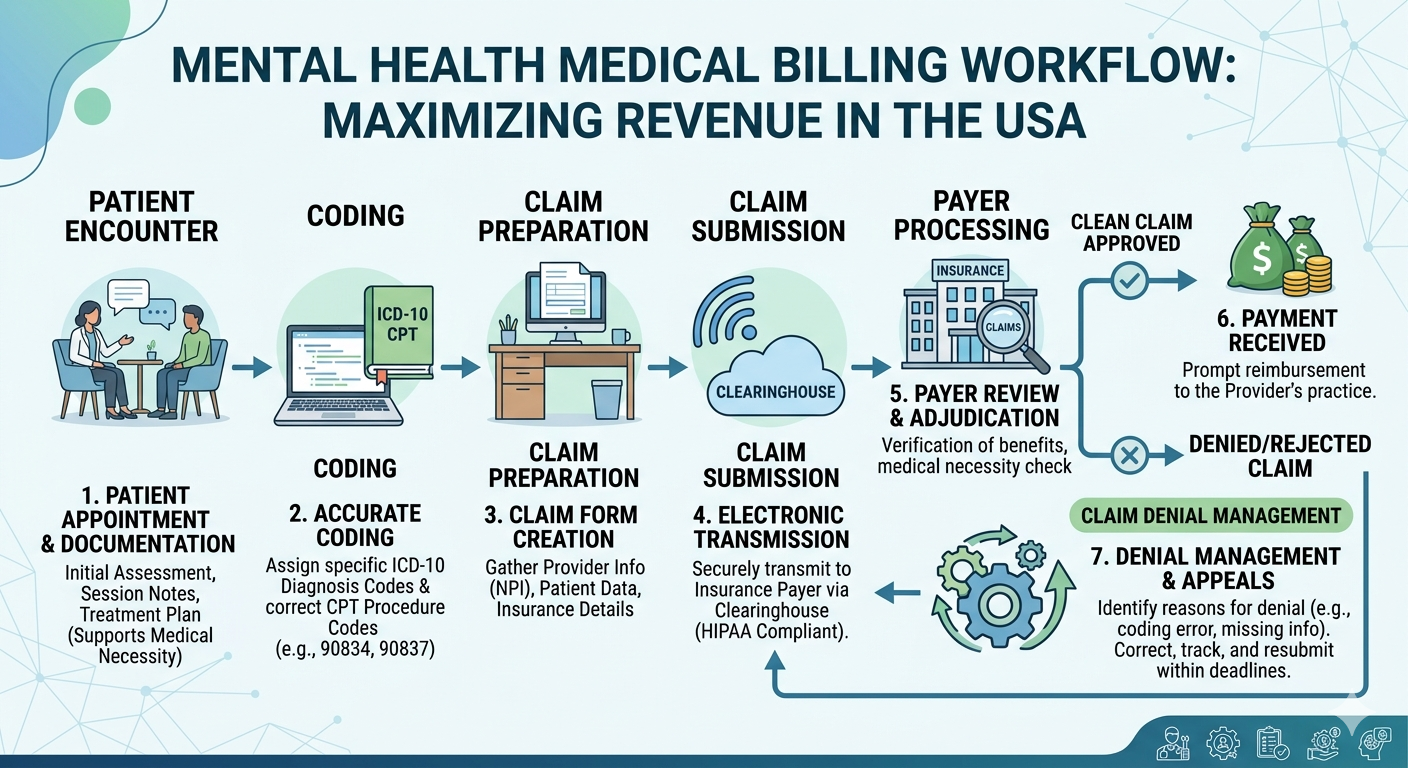
Mental health billing is not the same as general medical billing. It involves unique codes, session-based billing structures, and strict compliance requirements. From handling CPT codes for therapy sessions to navigating payer-specific guidelines, the margin for error is high.
Many providers attempt to manage billing in-house, only to face:
- Frequent claim denials
- Delayed reimbursements
- Coding inaccuracies
- Compliance risks
A dedicated mental health billing specialist understands these nuances and ensures every claim is submitted correctly the first time.
What Does a Mental Health Billing Services Company Actually Do?
A professional mental health billing services agency goes beyond just claim submission. It acts as a strategic partner that manages the entire financial workflow of your practice.
Here’s what they typically handle:
1. Insurance Verification & Eligibility Checks
Before a patient even steps into your office, verifying coverage is critical. Billing teams ensure benefits are active and sessions are reimbursable.
2. Accurate Coding
Using precise CPT and ICD-10 codes is crucial. A skilled mental health billing and coding company reduces errors that often lead to denials.
3. Claims Submission & Tracking
Claims are submitted promptly and tracked until payment is received—no more guessing or follow-ups falling through the cracks.
4. Denial Management
Denied claims are analyzed, corrected, and resubmitted quickly to recover lost revenue.
5. Payment Posting & Reporting
Detailed financial reports give you full visibility into your practice’s performance.
Why Providers Choose to Outsource Mental Health Billing Services
Outsourcing is no longer just a cost-saving tactic—it’s a growth strategy.
Reduced Administrative Burden
Managing billing in-house takes time away from patient care. With outsourced mental health billing, providers can focus entirely on clinical work.
Improved Revenue Cycle
Experienced teams streamline processes, leading to faster reimbursements and fewer denials.
Access to Expertise
A top outsource mental health billing company brings industry knowledge that’s difficult to replicate internally.
Scalability
As your practice grows, billing complexity increases. Outsourcing ensures your systems grow with you.
Key Features of the Best Mental Health Billing Agency
Not all billing partners are created equal. The best mental health billing agency will offer:
- Specialized experience in behavioral health
- Transparent reporting systems
- HIPAA-compliant workflows
- Dedicated account managers
- Custom solutions tailored to your practice size
Look for a partner that understands both the clinical and financial side of mental healthcare.
Real-World Example: Small Practice to Scalable Growth
Consider a mid-sized therapy clinic in Texas that struggled with inconsistent cash flow. They had an in-house billing assistant, but claim denials hovered around 25%.
After switching to a mental health medical billing solution, they saw:
- Denials drop to under 8%
- Revenue increase by 30% within six months
- Administrative workload cut in half
This isn’t an isolated case—many mental health billing companies deliver similar outcomes when processes are optimized.
How Mental Health Insurance Billing Services Improve Cash Flow
Insurance companies have strict rules, and even minor errors can delay payments. Professional mental health insurance billing services ensure:
- Clean claims submission
- Faster processing times
- Reduced rejections
- Accurate documentation
This directly impacts your bottom line and ensures steady revenue.
Billing Services for Mental Health Therapists: A Tailored Approach
Therapists face unique billing challenges, including session limits, telehealth regulations, and varying payer rules.
Specialized billing services for mental health therapists address:
- Individual vs. group therapy billing
- Teletherapy compliance
- Session-based reimbursement models
This level of customization is what separates general billing providers from true mental health experts.
The Role of Technology in Mental Health Medical Billing Services
Modern mental health medical billing services outsourcing leverages technology to enhance efficiency.
Key tools include:
- Automated claim scrubbing
- Real-time eligibility verification
- Advanced analytics dashboards
- Secure patient data systems
These tools not only reduce errors but also provide actionable insights into your practice’s financial health.
Revenue Cycle Management: The Bigger Picture
Billing is just one part of a larger system. Effective revenue cycle management services cover the entire patient journey—from appointment scheduling to final payment.
When integrated properly, it ensures:
- Faster billing cycles
- Better patient payment experiences
- Increased overall revenue
For mental health providers, this holistic approach is crucial for long-term sustainability.
Why Medical Coding Services Matter in Mental Health Billing
Accurate coding is the foundation of successful billing. Errors in coding can lead to compliance issues and lost revenue.
Professional medical coding services ensure:
- Correct diagnosis and procedure codes
- Compliance with insurance guidelines
- Reduced audit risks
When combined with medical billing and coding services, the entire process becomes seamless and efficient.
Credentialing: The Often Overlooked Revenue Driver
Many providers underestimate the importance of credentialing services. Without proper credentialing:
- Claims can be denied outright
- Providers may not be reimbursed
- Network participation is limited
A strong billing partner ensures credentialing is handled correctly, allowing you to maximize payer relationships.
Choosing the Right Mental Health Billing Agency
When evaluating a mental health billing agency, ask these questions:
- Do they specialize in behavioral health?
- What is their claim acceptance rate?
- How do they handle denials?
- What reporting tools do they offer?
Your billing partner should feel like an extension of your team—not just a vendor.
The Future of Mental Health Billing in the USA
As telehealth continues to expand and insurance policies evolve, billing will only become more complex. Practices that adapt early—by investing in professional mental health medical billing services—will have a clear advantage.
Outsourcing is no longer optional for many—it’s becoming the standard.
A Thoughtful Approach to Growth
If your goal is to grow your practice without burning out, outsourcing billing is one of the smartest decisions you can make. Whether you’re a solo therapist or managing a multi-location clinic, the right mental health billing services company can transform your operations.
Before wrapping up, it’s worth noting that providers often benefit from partners who offer a full suite of solutions—ranging from medical billing services and medical coding services to comprehensive medical billing and coding services, along with integrated revenue cycle management services and reliable credentialing services.
Companies like 247 medical billing services are often considered by practices looking for a balanced approach—where operational efficiency meets compliance and financial growth—without unnecessary complexity.
FAQs
1. What is a mental health billing services company?
A mental health billing services company specializes in handling billing, coding, and insurance processes specifically for behavioral health providers, ensuring accurate claims and faster reimbursements.
2. Why should I outsource mental health billing services?
Outsourcing reduces administrative workload, improves claim accuracy, speeds up payments, and allows providers to focus more on patient care.
3. How do mental health billing specialists reduce claim denials?
They use accurate coding, verify insurance details, and follow payer-specific guidelines to ensure claims are submitted correctly the first time.
4. Are billing services for mental health providers expensive?
Costs vary, but most practices find that outsourcing increases revenue enough to outweigh the expense, making it a cost-effective solution.
5. What is included in mental health medical billing services?
Services typically include insurance verification, coding, claims submission, denial management, payment posting, and reporting.
6. How do I choose the best mental health billing agency?
Look for experience in behavioral health, transparent reporting, strong client reviews, and a proven track record of reducing denials and increasing revenue.

